The Therapeutic Order in Heart Disease: A brief summary of evidence
February 11, 2020 | Evidence in Integrative Healthcare
February is designated by NIH as “heart health month.” St. Valentine’s Day, get it? As the website proclaims, “The annual celebration began in 1963 to encourage Americans to join the battle against heart disease.” In honor of National Heart Month, this blog post will focus on heart health from an Integrative Health (IH) perspective, specifically, that of Naturopathic Doctors (ND) and the substantial medical evidence that currently supports the “Therapeutic Order” of the ND approach.
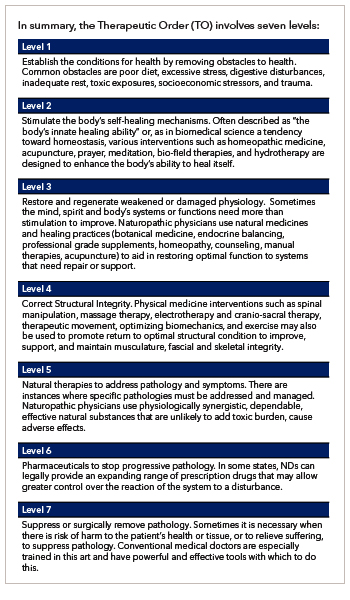 Central to the teaching, practice, and research in naturopathic medicine is the “Therapeutic Order (TO).” NDs have always espoused natural therapeutic interventions. This long-standing tradition evolved into the TO. First elaborated formally by Zeff in 19971Zeff J. The Process of Healing: A Unifying Theory of Naturopathic Medicine. Journal of Naturopathic Medicine 1997;7:122-5. and subsequently refined by others2Finnell J, Snider P, Myers S, Zeff J. A Hierarchy of Healing: Origins of the Therapeutic Order and Implications for Research. Integrative Medicine Vol. 18, No. 3 June 2019., the Therapeutic Order (TO) is the expression of the philosophy, “…that the human form possesses an inherent drive to heal itself. The least possible amount of force should be employed…” to benefit the patient.3American Association of Naturopathic Medicine Colleges. The therapeutic order. Aug 6, 2019.
Central to the teaching, practice, and research in naturopathic medicine is the “Therapeutic Order (TO).” NDs have always espoused natural therapeutic interventions. This long-standing tradition evolved into the TO. First elaborated formally by Zeff in 19971Zeff J. The Process of Healing: A Unifying Theory of Naturopathic Medicine. Journal of Naturopathic Medicine 1997;7:122-5. and subsequently refined by others2Finnell J, Snider P, Myers S, Zeff J. A Hierarchy of Healing: Origins of the Therapeutic Order and Implications for Research. Integrative Medicine Vol. 18, No. 3 June 2019., the Therapeutic Order (TO) is the expression of the philosophy, “…that the human form possesses an inherent drive to heal itself. The least possible amount of force should be employed…” to benefit the patient.3American Association of Naturopathic Medicine Colleges. The therapeutic order. Aug 6, 2019.
The “Therapeutic Order” emerged at roughly the same time as what came to be known as “Evidence Based Medicine (EBM)” was being developed. We will look at the Level 1 of the TO of naturopathic medicine but through the lens of EBM as it applies to ND prevention and management of heart disease. A brief selection of the current medical evidence that bears on the TO is cited.4Virani et a.l Heart Disease and Stroke Statistics—2020 Update. Circulation. 2020;141:00–00. DOI: 10.1161/CIR.0000000000000757 It is clear that the TO can be, and likely is, evidence based.
So let’s take a look at the Level 1 in the TO to see what some of the current best medical evidence says about the naturopathic medicine approach to heart health.
Level 1 in the TO is to “Remove obstacles to health. Common obstacles are poor diet, excessive stress, digestive disturbances, inadequate rest, toxic exposures, socioeconomic stressors, and trauma.” Breaking all of these down in detail is well beyond the scope of this blog post, but a high level overview of these obstacles clearly identifies most of the risk factors and preventive measures that can manage the threat of heart disease in the population. The NDs are right on it!
| Therapeutic Order - Level 1 | Brief sample of the current evidence |
|---|---|
| Poor diet | DASH Diet DASH stands for Dietary Approaches to Stop Hypertension (DASH) is an eating plan based on research studies sponsored by the National Heart, Lung, and Blood Institute (NHLBI). (National Heart, Lung, and Blood Institute. https://www.nhlbi.nih.gov/health-topics/dash-eating-plan) Adherence to a Mediterranean-style dietary pattern was associated with lower all-cause mortality in individuals with CVD. (Lopez-Garcia E, Rodriguez-Artalejo F, Li TY, et al. The Mediterranean-style dietary pattern and mortality among men and women with cardiovascular disease. Am J Clin Nutr. 2014;99(1):172–180. doi:10.3945/ajcn.113.068106) |
| Excessive stress | There are growing amounts of evidence supporting a role for job strain, effort‐reward imbalance, and organizational injustice contributing to CHD. (Sara JD, Prasad M, Eleid MF, Zhang M, Widmer RJ, Lerman A. Association Between Work-Related Stress and Coronary Heart Disease: A Review of Prospective Studies Through the Job Strain, Effort-Reward Balance, and Organizational Justice Models. J Am Heart Assoc. 2018;7(9):e008073. Published 2018 Apr 27. doi:10.1161/JAHA.117.008073) |
| Digestive disturbances | Helicobacter pylori (cause of stomach ulcers) has been recently introduced as an important etiological factor for heart disease. (Jamkhande PG, Gattani SG, Farhat SA. Helicobacter pylori and cardiovascular complications: a mechanism based review on role of Helicobacter pylori in cardiovascular diseases. Integr Med Res. 2016;5(4):244–249. doi:10.1016/j.imr.2016.05.005) |
| Inadequate rest | Both short sleep duration and poor sleep quality are associated with the risk of coronary heart disease. ( Lao XQ, Liu X, Deng HB, et al. Sleep Quality, Sleep Duration, and the Risk of Coronary Heart Disease: A Prospective Cohort Study With 60,586 Adults. J Clin Sleep Med. 2018;14(1):109–117. Published 2018 Jan 15. doi:10.5664/jcsm.6894) |
| Toxic exposures | Literature reviews done by the US Environmental Protection Agency, WHO, and others have shown that long-term exposure to ambient air pollution increases mortality and morbidity from cardiovascular and respiratory disease and lung cancer and shortens life expectancy. ( Cohen AJ, Brauer M, Burnett R, et al. Estimates and 25-year trends of the global burden of disease attributable to ambient air pollution: an analysis of data from the Global Burden of Diseases Study 2015 [published correction appears in Lancet. 2017 Jun 17;389(10087):e15] [published correction appears in Lancet. 2018 Apr 21;391(10130):1576]. Lancet. 2017;389(10082):1907–1918. doi:10.1016/S0140-6736(17)30505-6) |
| Socioeconomic stressors | Financial stress may be an unrecognized risk factor for coronary heart disease (Moran K, et.al. Financial Stress and Risk of Coronary Heart Disease in the Jackson Heart Study. Am J Prev Med. 2019 Feb;56(2):224-231. doi: 10.1016/j.amepre.2018.09.022) |
| Trauma | Trauma exposure and elevated PTSD symptoms may increase the risk of CVD in this population of women. ( Sumner J, et.al. Trauma Exposure and Posttraumatic Stress Disorder Symptoms Predict Onset of Cardiovascular Events in Women. Circulation. 2015;132:251–259.) We found a dose-response relation of Adverse Childhood experiences (ACEs) to ischemic heart disease(IHD) and a relation between almost all individual ACEs and IHD. (Dong M, Giles WH, Felitti VJ, Dube SR, Williams JE, Chapman DP, Anda RF. Insights into causal pathways for ischemic heart disease: adverse childhood experiences. Circulation. 2004;13(13):1761–1766. doi: 10.1161/01.CIR.0000143074.54995.7F) |
The medical evidence that supports the ideas that “…poor diet, excessive stress, digestive disturbances, inadequate rest, toxic exposures, socioeconomic stressors, and trauma…” all contribute to heart disease is over whelming. While some of the common preventive heart health recommendations have not been studied in randomized controlled clinical trials, some do have high levels of evidence and are univocally promoted by expert clinical authorities.